Lung
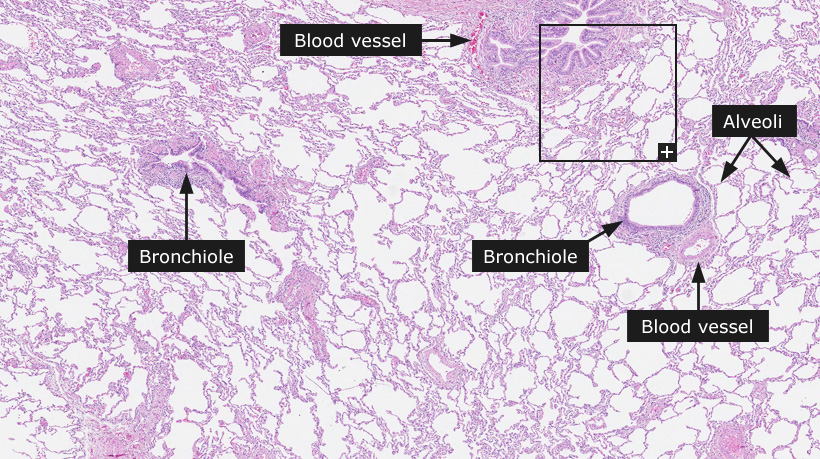
Lung
The principle function of the lung is to provide oxygen to the blood and in exchange rid the blood from carbon dioxide. The main cell types of the bronchioles are similar to that seen in the bronchus namely, basal cells, neuroendocrine cells, ciliated cells, serous cells, Clara cells and goblet cells. Goblet and ciliated cells decrease in number as one approaches the terminal bronchioles, whereas the number of Clara cells increases proportionally. The Clara cells have a secretory function and represent the main progenitor cell after bronchiolar injury. They are columnar to cuboidal in shape and project above the ciliated cells into the airway lumen.
The pulmonary alveoli are demarcated by septa composed of a continuous layer of epithelial cells overlying a thin interstitium. Two morphologically distinct cells - type I and type II (granular) pneumocytes (alveolar cells) line the alveoli. Alveolar macrophages are also present on the epithelial surface. The interstitium contains capillaries involved in gas exchange, as well as connective tissue and a variety of cells involved in alveolar shape and defense.
Type 1 pneumocytes cover approximately 95% of the alveolar septal surface. The nucleus is small and is covered by a thin rim of cytoplasm. The rest of the cytoplasm extends as a broad sheet over the alveolar surface. Adjacent type 1 pneumocytes are joined to one another by tight junctions that provide a barrier to the diffusion of water soluble substances into the alveolar airspace. Type 2 pneumocytes tend to be located near the alveolar intersections and exhibit a granular cytoplasm. Type 2 pneumocytes have several important functions, including the production of surfactant responsible for modifying alveolar surface tension. These cells also have the ability to be mitotically active and differentiate into type 1 cells, and synthesize substances such as fibronectin and α-1-antitrypsin that are involved in alveolar structure and defense, and enhancement of macrophage function.
Cancer: Lung cancer
|